
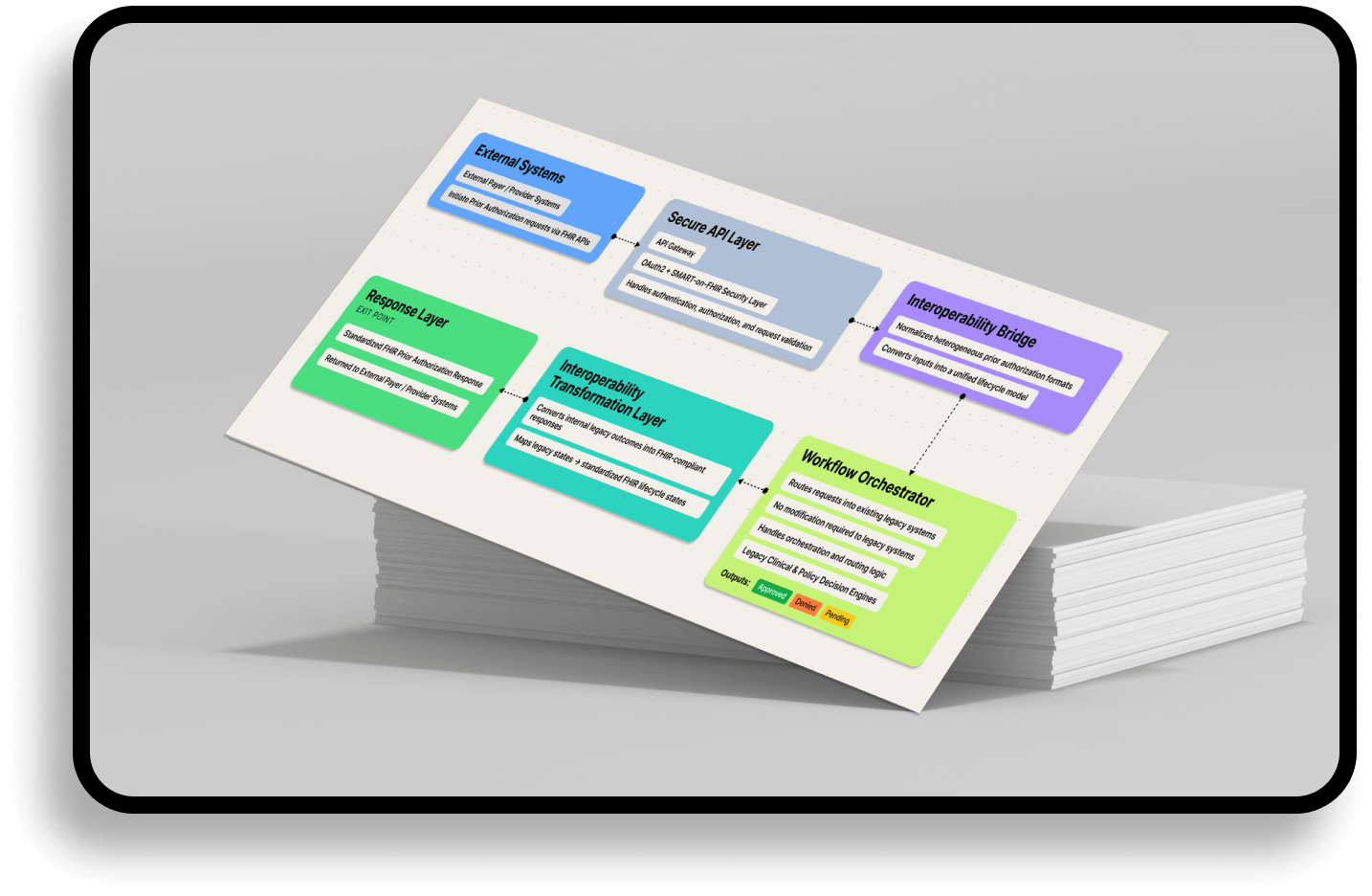
A U.S. healthcare clearinghouse engaged CleverDev Software to design and implement a FHIR-based interoperability enablement layer for CMS-0057-F readiness.
The objective was to introduce FHIR Prior Authorization APIs and an interoperability bridge that could operate alongside legacy transaction systems without disrupting production workflows.
Within a 6-month delivery window, CleverDev Software delivered:
This created a FHIR-compatible integration layer for prior authorization workflows while preserving existing system behavior.
The client is a U.S. healthcare clearinghouse responsible for routing eligibility, claims, and prior authorization transactions between payors and providers.
While operational systems were stable, prior authorization workflows were fragmented across multiple internal systems, limiting real-time visibility for payor partners.
At the same time, payor organizations were increasingly expecting FHIR-based prior authorization APIs aligned with CMS interoperability direction.
CMS-0057-F is a Centers for Medicare & Medicaid Services interoperability rule that modernizes prior authorization using HL7 FHIR standards. FHIR enables standardized, API-based healthcare data exchange, complementing existing legacy workflows.
The rule drives the industry toward:
While compliance deadlines extend into 2026–2027, payor expectations are already shifting toward FHIR-first integration models.
The core challenge was not API development — it was inconsistent prior authorization state representation across systems.
Different internal systems interpreted authorization status differently:
This made it difficult to expose reliable FHIR-based prior authorization APIs without normalization.
Additional constraints included:
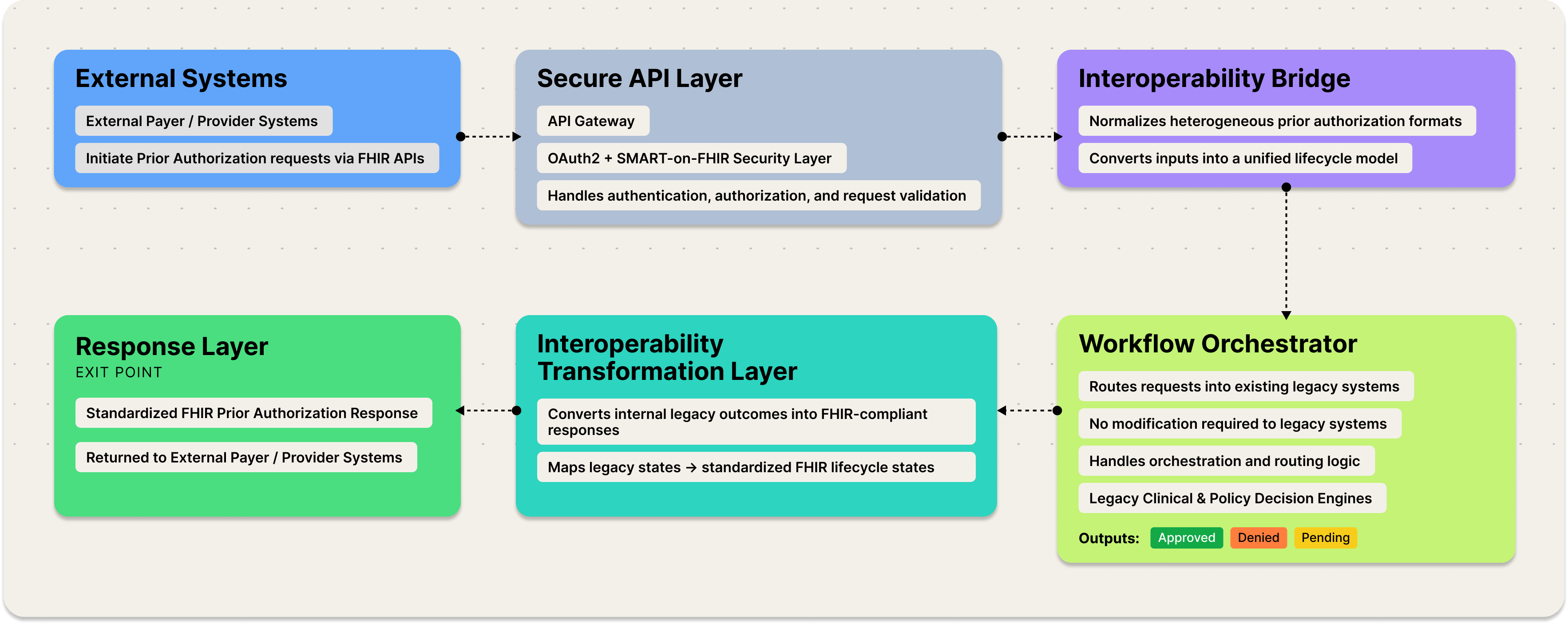
The architecture introduced a FHIR interoperability enablement layer designed to sit above legacy systems.
Standardized APIs for:
This enabled external FHIR-based API integrations without impacting internal workflows.
A transformation layer that maps internal workflow states into FHIR-compatible representations at request time. This mapping is deterministic but does not enforce a canonical lifecycle model across systems.
Instead of polling-based status checks, the system used:
This enabled near real-time prior authorization status updates.
A lightweight event log enabling:
This layer supports operational observability but does not provide a complete, system-of-record audit history.
The delivery followed a phased interoperability approach.

The clearinghouse deployed a FHIR-compatible prior authorization interface within 6 months while maintaining uninterrupted existing operations:
The solution provides a pragmatic compliance layer for CMS-0057-F readiness, enabling external integrations without requiring immediate re-platforming of legacy systems.
If your organization is implementing HL7 FHIR R4-based prior authorization APIs, planning for CMS-0057-F, or exposing legacy workflows through modern interfaces, CleverDev Software supports pragmatic, low-risk approaches to healthcare integrations aligned with real system constraints.
We work with healthcare clearinghouses, payors, and RCM platforms to design and deliver:
Our focus is on enabling compliance and external interoperability without requiring immediate re-platforming of core systems.

